Diabetic Retinopathy
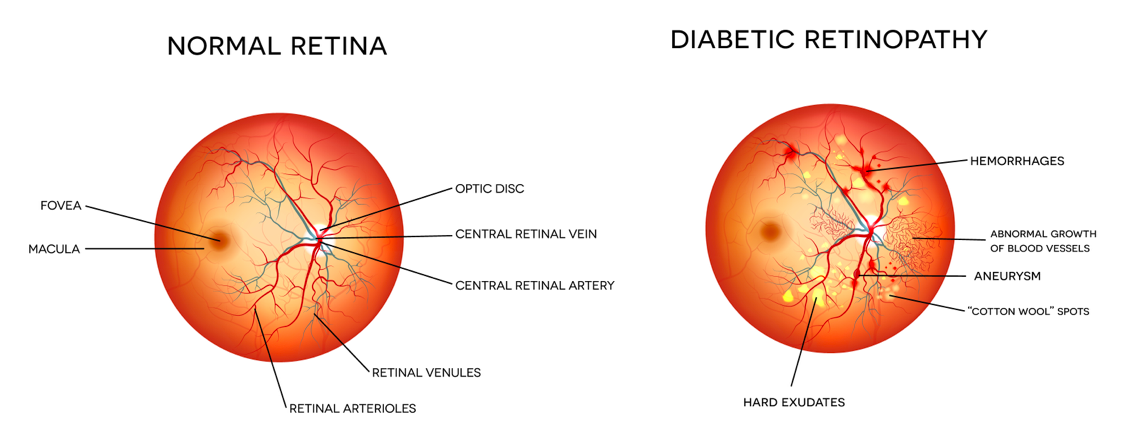
What causes it?
Diabetic eye disease includes fluctuations in vision that can be related to changing blood glucose levels, as well as more sustained changes in vision from cataract and diabetic retinopathy.
Diabetic retinopathy is a term used to describe the changes that are seen in the retina of people with diabetes.
High blood sugar levels cause damage to the small blood vessels in the retina, which can lead to bleeding and swelling of the retina, as well as the growth of abnormal new blood vessels and scar tissue. These changes develop over time, but are likely to develop sooner, or be more severe, if blood glucose levels are not well controlled.
In its early stages, diabetic retinopathy does not usually cause any symptoms, so you may not even know you have it.
Regular eye examinations are a key part of your diabetes care, so that diabetic retinopathy can be detected and treated before you notice any changes in your vision. Management of diabetic retinopathy is very effective and can often slow the progression of the disease. By the time diabetic retinopathy causes symptoms, it is often severe and more difficult to treat.
How to check for the condition
A full diabetic eye examination, should be performed at the time of diagnosis of diabetes and at least once every 1 year thereafter. More frequent eye checks may be needed for people with existing diabetic retinopathy and for people at high risk of progressive disease, including those who have had diabetes for many years or those with other complications of diabetes (such as kidney disease or neuropathy).
The optometrist will check your vision and then check the retina to look for any retinopathy. Your eye health will be comprehensively assessed.
Eye drops may be used to examine your eyes in a diabetic eye examination – these can temporarily blur your vision. It is advised not to drive for up to 2 hours after your drops.
Cataracts develop over many years and problems may at first be unnoticeable. They often develop in both eyes, although each eye may be affected differently. You will usually have blurred, cloudy or misty vision. You may find it more difficult to see in dim or very bright light. Bright lights may be dazzling or uncomfortable to look at and colours may look faded or less clear with a yellow or brown tinge. You may see haloes (circles of light) around bright lights, such as car headlights or street lights
